7 results
2 Neuropsychological Test Performance Following Acute COVID-19 Infection Recovery: A Case Control Study
- Theone S. E. Paterson, Kristina M Gicas
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 875-876
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Cognition has been identified as an area of priority in examining health impacts of COVID-19 infection, and evidence suggests the virus invades the brain, with potential for long-term cognitive impact. Studies utilizing screening measures have reported cognitive sequelae (e.g., attention disorder, executive dysfunction) of the post-COVID-19 condition (i.e., long-haulers). More extensive examination of cognitive difficulties via comprehensive neuropsychological assessment is critical to informing treatment for those experiencing cognitive or functional difficulties post-infection. We aimed to comprehensively evaluate cognitive resiliencies and vulnerabilities of acutely recovered COVID-19 patients, across key domains (i.e., attention, processing speed, language, visuospatial abilities, memory, executive functioning), compared to healthy controls.
Participants and Methods:Adults (N=103; aged 19-85; 69.2% female) who had COVID-19 at least three months prior (n=50) and those with no history of infection (n=53) completed demographic and health questionnaires via Qualtrics, along with measures of depressive (CES-D) and anxiety (GAD-7) symptoms, the Lawton-Brody Instrumental Activities of Daily Living (IADL) Scale, and a measure of subjective cognitive difficulties (SCD-Q). Participants (n=84) completed a teleneuropsychology assessment including a short interview and battery of neuropsychological tests assessing attention (BTA, Digit Span Forward), processing speed (DKEFS Colour Naming & Word Reading, SDMT), language (FAS, Animals, NAB Naming), visuospatial abilities (JLO, RCFT Copy), verbal and visual memory (HVLT-R, NAB Shape Learning, RCFT), and executive function (DKEFS Color-Word Interference & Switching, Digit Span Backward & Sequencing, BRIEF), and including multiple measures of cognitive effort/assessment validity (RFIT, RDS), and a self-report measure of symptom validity (SIMS). T-tests were used to examine demographic and health variables between COVID-19 and control groups. MANCOVA were used to examine group differences across each cognitive domain assessed, and across cognitive effort and symptom validity tasks, while controlling for English language status.
Results:Group comparisons indicated that the COVID-19 group was slightly older (mean age = 40 vs. 34 yrs.; f=-2.101, p=0.04). Those who had COVID-19 reported more difficulties completing IADLs (f=2.204; p=0.03), more depressive symptoms (f=-2.299; p=0.02), and more subjective cognitive difficulties (f=-3.886; p<0.01). Examination of cognitive performance indicated a main effect of prior infection on executive function, controlling for language status (Wilks’ /\=0.817, F(6,73)=2.733, p=0.02). Specifically, having COVID-19 was associated with worse DKEFS Colour-Word Switching performance (p=0.01) and slightly higher selfreported difficulties on the BRIEF MI (p=0.04). No other significant group differences were seen across cognitive domains. There was also a main effect of COVID-19 infection on effort and symptom validity task performance (Wilks’ /\=0.705, F(10,70)=2.923, p<0.01). Specifically, prior infection was associated with higher SIMS Neurologic Impairment (p<0.01) and Amnestic Disorders (p<0.01) subscale scores, and paradoxically, slightly higher RFIT combined scores (p=0.02).
Conclusions:Interestingly, results indicate a significant role for subjective cognitive complaints and potential exaggeration of cognitive symptoms post-COVID-19 infection, in the absence of differences in objective performance in most cognitive domains. While subtle differences are seen on some executive function measures, mean group differences are small, and in the context of higher SIMS subscale scores, may not be readily interpretable. Studies employing similarly comprehensive neuropsychological assessments including validity measures in larger samples are needed to further disambiguate potential objective cognitive performance decrements from subjectively experienced difficulties.
47 The Impact of COVID-19 Infection on Objective and Subjective Cognitive Functioning: Resilience as a Protective Factor
- Alexa M. Danyluk, Morgan J. Schaeffer, Laurel Caldwell-MacIntyre, Kristina M. Gicas, Theone S. E. Paterson
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 44-45
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Growing evidence indicates that COVID-19 infection adversely impacts cognitive functioning, with COVID-19 patients demonstrating high rates of objective and subjective cognitive impairments (Daroische et al., 2020; Miskowiak et al., 2021). Given the prevalence and potentially debilitating nature of post-COVID-19 cognitive symptoms, understanding factors that mitigate the impact of COVID-19 infection on cognitive functioning is paramount to developing interventions that facilitate recovery. Resilience, the ability to cope with and grow from challenges, has been associated with improved cognitive performance in healthy adults and linked to decreased perceived cognitive difficulties in post-COVID-19 patients (Connor & Davidson, 2003; Deng et al., 2018; Jung et al., 2021). However, resilience has not yet been examined as a potential attenuator of the relationship between COVID-19 and either perceived or objective cognitive function. This study aims to investigate the role of resilience as a protective factor against experience of cognitive function difficulties in COVID-19 patients by probing the role of resilience as a moderator of the relationship between COVID-19 diagnosis and cognitive functioning (both perceived and objective).
Participants and Methods:Participants (mean age=36.93, 30.10% male) were recruited from British Columbia and Ontario. The sample included 53 adults who had never been diagnosed with COVID-19 and 50 adults diagnosed with symptomatic COVID-19 at least three months prior and not ventilated. Participants completed online questionnaires (n=103) to assess depression (the Center for Epidemiological Studies Depression Scale), anxiety (7-item Generalized Anxiety Disorder Scale), subjective cognitive functioning (The Subjective Cognitive Decline Questionnaire), and resilience (2-item Connor-Davidson Resilience Scale). Participants then completed neuropsychological tests (n=82) measuring attention, processing speed, memory, language, visuospatial skills, and executive function via teleconference, with scores averaged to create a global objective cognition score. Moderated multiple regression was employed to assess the impact of resilience on the relationship between COVID-19 diagnosis and both objective and perceived cognition, controlling for gender, ethnicity, income, age, anxiety, and depression.
Results:Average scores in the COVID-19 group exceeded diagnostic cut-offs for clinical depression (M=16.67, SD=10.77) and mild anxiety (M=5.27, SD=4.99), while the control group scored below diagnostic thresholds for depression (M=11.96, SD=9.76) and mild anxiety (M=4.48, SD=5.07). Controlling for sociodemographic and mental health characteristics, COVID-19 diagnosis was not associated with objective global cognitive functioning (b=-.07, se=1.71, p=.624) or subjective cognitive functioning (b=.16, se=1.32, p=.12), nor was resilience associated with objective global cognitive functioning (b=.19, se=1.50, p=.44) or subjective cognitive functioning (b=-.02, se=1.09, p=.89).
Conclusions:Findings indicate that COVID-19 patients may be at risk for depression and anxiety. Results of this study fail to support a relationship between COVID-19 and cognitive functioning beyond the impact of sociodemographic and mental health variables. Thus, the role of resilience as a protective factor against COVID-19 related cognitive difficulties could not be fully explored. However, findings should be considered in the context of study limitations, including a small sample size. Future research should employ larger samples to further examine the relationship between COVID-19 infection and cognition, focusing on mental health characteristics and resilience as potential risk and protective factors.
52 Depressive Symptoms and Subjective Cognitive Decline in Individuals with COVID-19
- Eva Friedman, Petra Legaspi, Katie C Benitah, Samantha J Feldman, Theone S. E. Paterson, Kristina M Gicas
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 49-50
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Many individuals with COVID-19 develop mild to moderate physical symptoms that can last days to months. In addition to physical symptoms, individuals with COVID-19 have reported depressive symptoms and cognitive decline, posing a long-term threat to mental health and functional outcomes. Few studies have examined the presence of co-occurring depression and subjective cognitive decline in individuals who tested positive for COVID-19. The current study examined whether having COVID-19 is subsequently associated with greater depressive symptoms and subjective cognitive decline when compared to healthy individuals. Our study also examined differential associations between symptoms of depression and subjective cognitive decline between individuals who have and have never had COVID-19.
Participants and Methods:Adults (N = 104; mean age = 37 years, 69% female) were recruited online from Ontario and British Columbia, Canada. Participants were categorized into two groups: (1) persons who tested positive for COVID-19 at least three months prior, had been symptomatic, and had not been ventilated (N = 50); and (2) persons who have never been suspected of having COVID-19 (N = 54). The Center for Epidemiological Studies Depression Scale (CES-D) and the Subjective Cognitive Decline Questionnaire (SCD-Q) were administered to both groups as part of a larger clinical neuropsychological evaluation. Two separate linear regression analyses were conducted to examine the association of COVID-19 with depressive symptoms and subjective cognitive decline. A moderation analysis was performed to examine whether depressive symptoms were associated with subjective cognitive decline and the extent to which this differed by group (COVID-19 and controls). Participants’ age, self-reported sex, and history of depression were included as covariates.
Results:The first regression model explained 17.2% of the variance in CES-D scores. It was found that the COVID-19 group had significantly higher CES-D scores (ß = .20, p = .03). The second regression model explained 35.9% of the variance in SCD-Q scores. Similar to the previous model, it was found that the COVID-19 group had significantly higher SCD-Q scores compared to healthy controls (ß = .22 p = .01). Lastly, the moderation model indicated that higher CES-D scores were associated with higher SCD-Q scores (ß = .43, p < .01), but there was no statistically significant group X CES-D score interaction.
Conclusions:These findings suggest that individuals who previously experienced a mild to moderate symptomatic COVID-19 infection report greater depressive symptom severity as well as greater subjective cognitive decline. Additionally, while more severe depressive symptoms predicted greater subjective cognitive decline in our sample, the magnitude of this association did not vary between those with and without a previous COVID-19 infection. While the underlying neurobiological and social mechanisms of cognitive difficulties and depressive symptoms in persons who have had COVID-19 have yet to be fully elucidated, our findings highlight treatment for depression and cognitive rehabilitation as potentially useful intervention targets for the post COVID-19 condition.
The effect of chronobiology on frontal functions and social functionality in remitted patients with schizophrenia
- B. Çınar, S. Gıca, N. Karamustafalıoğlu
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S238
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Due to the effects of sleep on the central nervous system,it is thought that sleep problems have a special importance in the onset, course and treatment of psychiatric diseases. Although the negative effects of sleep problems on the occurrence, recurrence and clinical course of psychiatric disorders are well known, it is reported that clinicians do not spend enough time for sleep problems in practice.To our knowledge there is no study in the literature which examining its effect on frontal lobe functions or social functionality in schizophrenia.
ObjectivesIn current study, it is aimed i- to examine the chronobiological characteristics of remitted patients with schizophrenia, ii- to determine the effect of chronobiology on sleep quality, frontal lobe functions, depressive symptoms, interpersonal relationships and social functionality in patients with schizophrenia, iii- thus to improve the quality of life and the treatment outcome of patients with schizophrenia.
Methods185 patients with schizophrenia who met the Andreason remission criteria were included in the study. The patients were evaluated with Positive and Negative Syndrome Scale (PANSS), Morningness & Eveningness Scale (MEQ), Calgary Depression Index (CDI), Pitssburgh Sleep Quality Index (PSQI), Barratt Impulsivity Scale Short Form (BIS-11-SF), Frontal Assessment Battery (FAB), Personal Social Performance Scale (PSPS). Each patient was classified either as morning type (MT) or evening type (ET) or intermediate type (IT) according to MEQ scores.
ResultsThe obtained MEQ responses indicated that 29 (15.7%) of the patients were “ET”, 124 (67.0%) were “IT”, and 32 (17.3%) were “MT”. In the “ET” group, the mean of CDI total score, the mean of PSQI total score, the mean of BIS-11-SF total and the mean score of BIS-11-SF planlessness and inattention subscale were higher than in both the “IT” and “MT”. The mean total scores PSPS of “ET” patients were found to be lower than the mean scores of both the “IT” and “MT” patients. There was no significant difference between the groups in terms of FAB total scores. According to Multiple Linear Regression Analysis, total MEQ score and PANSS-negative symptoms subscale score were found to have an effect on PSPS[1]Personal Social Realitionship subscale scores.
ConclusionsAlthough all patients included in current study were in remission, it was found that chronotype characteristics were effective on many clinical manifestations and comorbid conditions. The findings obtained from our study emphasize how important it is to question chronotypic features in daily psychiatric practice. In this context, being aware of the importance of chronotypic features in the treatment of schizophrenia patients, questioning the patients in this respect and taking necessary interventions may have the potential to improve functionality, which is one of the main treatment goals in patients with schizophrenia.
Disclosure of InterestNone Declared
Longitudinal change in serial position scores in older adults with entorhinal and hippocampal neuropathologies
- Kristina M. Gicas, William G. Honer, Sue E. Leurgans, Robert S. Wilson, Patricia A. Boyle, Julie A. Schneider, David A. Bennett
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue 6 / July 2023
- Published online by Cambridge University Press:
- 05 September 2022, pp. 561-571
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
Serial position scores on verbal memory tests are sensitive to early Alzheimer’s disease (AD)-related neuropathological changes that occur in the entorhinal cortex and hippocampus. The current study examines longitudinal change in serial position scores as markers of subtle cognitive decline in older adults who may be in preclinical or at-risk states for AD.
Methods:This study uses longitudinal data from the Religious Orders Study and the Rush Memory and Aging Project. Participants (n = 141) were included if they did not have dementia at enrollment, completed follow-up assessments, and died and were classified as Braak stage I or II. Memory tests were used to calculate serial position (primacy, recency), total recall, and episodic memory composite scores. A neuropathological evaluation quantified AD, vascular, and Lewy body pathologies. Mixed effects models were used to examine change in memory scores. Neuropathologies and covariates (age, sex, education, APOE e4) were examined as moderators.
Results:Primacy scores declined (β = −.032, p < .001), whereas recency scores increased (β = .021, p = .012). No change was observed in standard memory measures. Greater neurofibrillary tangle density and atherosclerosis explained 10.4% of the variance in primacy decline. Neuropathologies were not associated with recency change.
Conclusions:In older adults with hippocampal neuropathologies, primacy score decline may be a sensitive marker of early AD-related changes. Tangle density and atherosclerosis had additive effects on decline. Recency improvement may reflect a compensatory mechanism. Monitoring for changes in serial position scores may be a useful in vivo method of tracking incipient AD.
Increase in brain connectivity with methylphenidate treatment in boys diagnosed with attention deficit hyperactivity disorder: A coherence-based qeeg analysis
- F.H. Çetin, Ş. Gıca, M. Çıkılı Uytun, Z. Babadağı, M.B. Usta, A.S. Güven, Y. Işık
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S634-S635
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Attention deficit hyperactivity (ADHD) disorder is a common childhood neurodevelopmental disorder, and Methylphenidate (MPH) is a first-line therapeutic option for treating ADHD.However, how brain connectivity changes with methylphenidate treatment have yet to be studied.
ObjectivesThis study investigates how the MPH treatment affects the connectivity in the brain of children with ADHD by coherence-based qEEG analysis during rest.
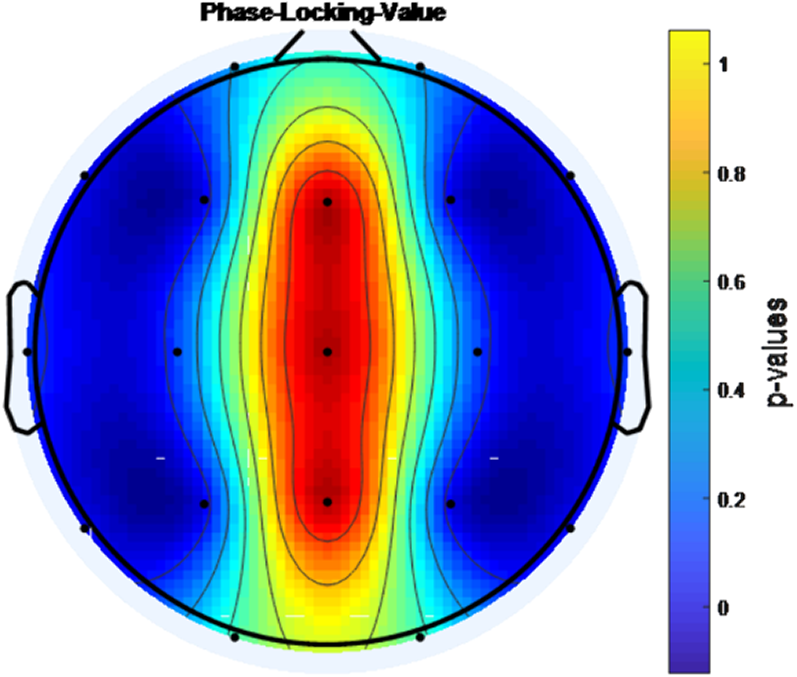
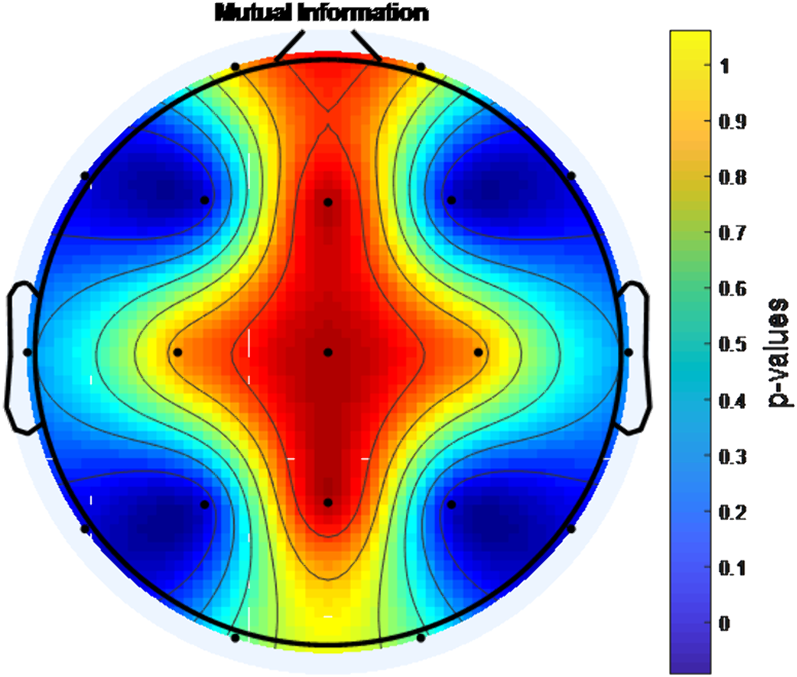
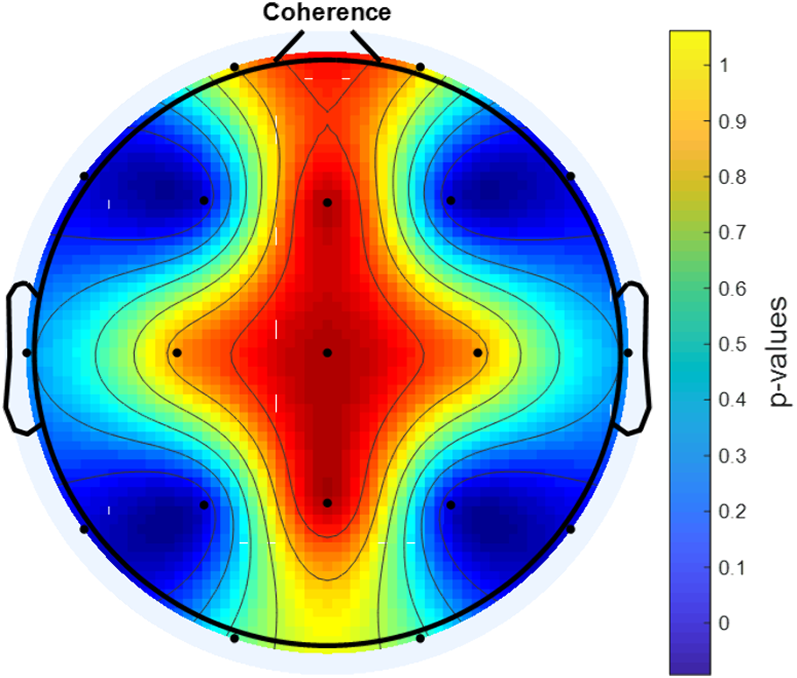
MethodsDuring eyes-open resting, EEG signals were recorded from 25 boys with ADHD-combined type before MPH administration and at the end of the 1st month of the treatment. Mutual Information (MI),Coherence Function (COH) and Phase Locking Value (PLV) were used to analyse the changes in brain connectivity.
ResultsA statistically significant increase in connectivity level was found with MPH treatment between the F3-F4 channels, P3-P4 channels, F7-F8 channels and T5-T6 channels according to PLV, COH and MI analysis (p<0.001).
 Conclusions
ConclusionsThis is the first study to investigate how MPH treatment affects the connectivity of the brain of children with ADHD. Coherence-based qEEG analysis may be a new method that can be used in diagnostic, clinical and prognostic predictions in ADHD.
DisclosureNo significant relationships.
Cognitive determinants of community functioning and quality of life in homeless adults with mental illness: 6-year follow-up from the At Home/Chez Soi Study Toronto site
- K. M. Gicas, C. Mejia-Lancheros, R. Nisenbaum, R. Wang, S. W. Hwang, V. Stergiopoulos
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 2 / January 2023
- Published online by Cambridge University Press:
- 30 April 2021, pp. 362-370
-
- Article
- Export citation
-
Background
High rates of physical and mental health comorbidities are associated with functional impairment among persons who are homeless. Cognitive dysfunction is common, but how it contributes to various functional outcomes in this population has not been well investigated. This study examines how cognition covaries with community functioning and subjective quality of life over a 6-year period while accounting for the effects of risk and protective factors.
MethodsParticipants were 349 homeless adults (mean age = 39.8) recruited from the Toronto site of the At Home/Chez Soi study, a large Canadian randomized control trial of Housing First. Participants completed up to four clinical evaluations over 6 years. Factor scores were created to index verbal learning and memory (vLM) and processing speed-cognitive flexibility (PSCF). The primary outcomes were community functioning and subjective quality of life. Risk factors included lifetime homelessness, mental health diagnoses, medical comorbidity, and childhood adversity. Linear mixed-effects models were conducted to examine cognition-functional outcome associations over time, with resilience as a moderator.
ResultsBetter vLM (b = 0.787, p = 0.010) and PSCF (b = 1.66, p < 0.001) were associated with better community functioning, but not with quality of life. Resilience conferred a protective effect on subjective quality of life (b = 1.45, p = 0.011) but did not moderate outcomes.
ConclusionsOur findings suggest a need to consider the unique determinants of community functioning and quality of life among homeless adults. Cognition should be prioritized as a key intervention target within existing service delivery models to optimize long-term functional outcomes.






